You probably don't think about your nervous system very often. But it's been thinking about you, all day, every day, deciding whether the world is safe or threatening before your conscious mind even registers the question. And for most people living modern lives, saturated by notifications, deadlines, and an endless scroll of bad news, that system has been stuck in the wrong gear for months or even years.
Welcome to the wellness conversation that's taken over 2026. Not a new supplement. Not a workout protocol. The nervous system itself, and the growing body of research suggesting we can actively train it to stop treating Tuesday morning emails like a bear attack.
Why "Just Relax" Never Works
The advice is familiar. Take a deep breath. Go for a walk. Practice gratitude. None of it is wrong, exactly, but it misses something fundamental about how stress actually operates in the body. The autonomic nervous system, which governs heart rate, digestion, immune response, and dozens of other involuntary functions, doesn't take orders from your rational brain. You can't think your way out of a racing heart any more than you can will your pupils to dilate.
This is the core insight driving the nervous system regulation movement: stress isn't just a feeling you experience. It's a physiological state your body enters, and it requires physiological tools to exit. Dr. Stephen Porges, whose polyvagal theory has shaped much of this conversation, frames it in terms of "neuroception," the body's unconscious surveillance system that constantly scans for safety or danger. When neuroception detects threat, whether from a snarling dog or a passive-aggressive Slack message, it triggers the same cascade of cortisol and adrenaline.
The problem isn't that this system exists. It kept our ancestors alive. The problem is that modern life rarely gives it the all-clear signal to stand down. Dr. Tiffany Field, director of the Touch Research Institute at the University of Miami, has spent decades studying how chronic low-grade stress alters autonomic function. "What we're seeing is that many people are living in a state of sympathetic dominance without realizing it," she told the Global Wellness Summit in January. "Their baseline has shifted. They think feeling wired and tired is normal."
The Vagus Nerve: Your Built-In Reset Button
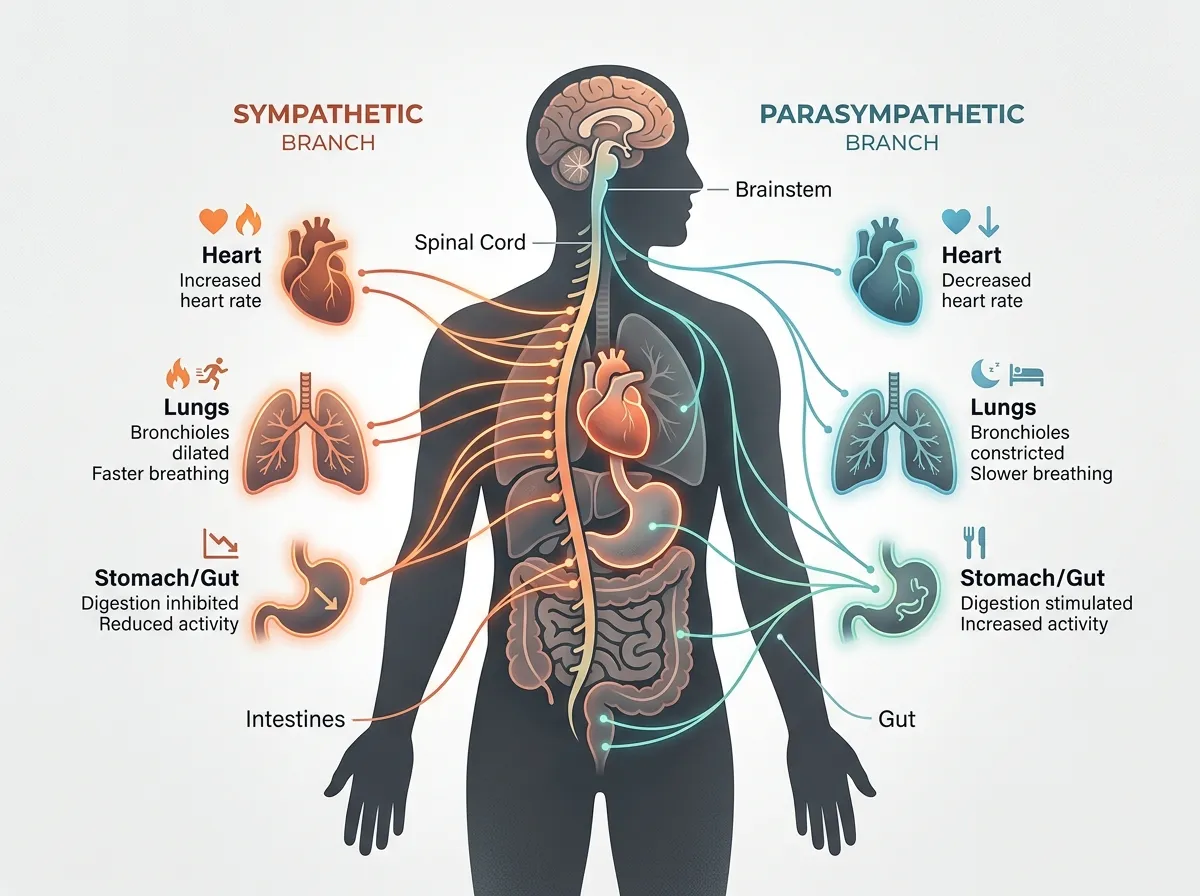
If the nervous system regulation trend has a star player, it's the vagus nerve. Running from the brainstem down through the neck, chest, and abdomen, the vagus nerve is the longest cranial nerve in the body and the primary communication highway between the brain and the gut, heart, and lungs. When it fires strongly, heart rate slows, inflammation decreases, digestion improves, and the body shifts into parasympathetic mode, the "rest and digest" state that allows recovery.
Researchers measure this activity through heart rate variability (HRV), the subtle variation in time between heartbeats. Higher HRV generally indicates a nervous system that can flex between activation and calm. Lower HRV is associated with chronic stress, cardiovascular disease, depression, and weakened immune function. A 2025 review published in Medicine International found that HRV biofeedback, where participants practice breathing at their individual resonance frequency while monitoring real-time heart data, significantly improved autonomic balance and reduced both anxiety and inflammatory markers across multiple clinical trials.
This is where the trend gets practical. Unlike many wellness fads that require expensive equipment or radical lifestyle changes, vagal tone can be improved with tools most people already have access to: their own breath.
The Science of Slow Breathing
The most extensively studied technique for nervous system regulation is also the simplest. Slow, deliberate breathing at roughly six breaths per minute activates the vagus nerve through a mechanism called respiratory sinus arrhythmia, where heart rate naturally rises during inhalation and falls during exhalation. By extending the exhale, you amplify the parasympathetic signal.
A study published in Scientific Reports found that a single session of slow, deep breathing produced measurable improvements in vagal tone in both young and older adults, with the effects appearing within minutes. The researchers noted that "longer exhalation times were associated with significantly greater increases in high-frequency HRV," the band most closely linked to parasympathetic activity. What's remarkable is how quickly the body responds. You don't need a meditation retreat or a six-week course. The physiological shift begins in the first few breaths.
This partly explains why breathwork has exploded in 2026. Apps like Othership, Breathwrk, and the Huberman-affiliated "Physiological Sigh" protocol have collectively seen downloads increase by over 300% since January, according to data from Sensor Tower. Wearable companies like Whoop, Oura, and Apple Watch have added dedicated nervous system recovery metrics to their dashboards. Even corporate wellness programs, traditionally focused on gym memberships and step challenges, are pivoting toward what the Global Wellness Summit calls "nervous system literacy."

What Actually Works (and What's Just Marketing)
Not everything sold under the "nervous system regulation" banner is backed by evidence. The market has flooded with vagus nerve stimulation devices, weighted blankets marketed as "parasympathetic activators," and $200 courses promising to "heal your dysregulated nervous system in 30 days." Some of it is useful. Much of it is over-optimization dressed up as self-care.
The evidence-supported interventions fall into a few categories. Breathwork, particularly slow breathing with extended exhales, has the strongest research base. Cold exposure, such as cold showers or ice baths, reliably activates the vagus nerve, though the effect is acute rather than cumulative. Humming and chanting stimulate the vagus through vibration of the larynx. Physical touch, including massage and even self-massage of the neck and ears, has been shown in Dr. Field's research to shift autonomic balance toward parasympathetic dominance.
What the science doesn't support is the idea that you need to buy your way into regulation. Dr. Rangan Chatterjee, author of "Feel Better in 5" and a vocal proponent of nervous system health, has been blunt about this on his podcast: "The most powerful vagal stimulation tool is free, available right now, and you've been doing it since birth. It's your breath. Everything else is an accessory."
The polyvagal framework that underpins much of this movement has also drawn legitimate scientific criticism. Neuroanatomists have challenged specific claims about vagal pathways, and some researchers argue the theory is too broad to test rigorously. But even critics acknowledge that the practical applications, breathwork, co-regulation, creating environments of safety, produce real clinical benefits regardless of whether the underlying neuroanatomy is precisely as Porges describes it.
The Cognitive Overload Connection
The nervous system conversation doesn't exist in a vacuum. It's rising alongside a broader recognition that modern life imposes an unsustainable cognitive load on the human brain. The constant context-switching between apps, the ambient anxiety of a 24-hour news cycle, the pressure to be perpetually available: these aren't just annoying. They're keeping millions of nervous systems locked in a state of chronic vigilance.
This is the original analysis that most coverage of the trend misses. Nervous system regulation isn't just about feeling calmer in the moment. It's a response to a structural problem in how we've organized daily life. The industrial economy demanded physical endurance. The knowledge economy demanded cognitive focus. The attention economy demands something different entirely: the ability to metabolize an endless stream of stimulation without breaking down. And that capacity lives in the autonomic nervous system.
Consider the data. A 2025 American Psychological Association survey found that 76% of adults reported physical symptoms of stress, up from 67% in 2019. Sleep tracker data from Oura's annual report shows average HRV declining across every age group for the third consecutive year. Emergency room visits for panic attacks among adults under 35 have increased 40% since 2020, according to CDC data. The nervous system isn't a wellness trend. It's a health crisis wearing a trendy hat.
What makes 2026 different from previous years isn't the problem. It's the shift in framing. People are moving past the idea that stress is a mindset issue you can journal your way out of and toward the recognition that it's a biological state requiring biological intervention. That shift matters because it removes the moral dimension from stress management. You're not failing at relaxation. Your hardware is stuck in a loop, and it needs a specific input to break free.

Start Here
If you want to experiment with nervous system regulation without buying anything or subscribing to anyone's program, start with what the research supports most strongly.
Try the "physiological sigh" protocol that Stanford neuroscientist Dr. Andrew Huberman has popularized: two quick inhales through the nose followed by one long exhale through the mouth. Research from his lab found this pattern reduced self-reported stress faster than box breathing, meditation, or mindfulness techniques in a randomized controlled trial. Do it two or three times when you notice tension building, not as a scheduled practice but as a real-time intervention.
Track your HRV if you have a wearable. Don't obsess over daily numbers, but watch for trends over weeks. A rising baseline suggests your nervous system is gaining flexibility. A declining baseline is worth paying attention to, especially if you're sleeping enough and not overtraining.
Most importantly, stop treating calm as something you earn after finishing your to-do list. The nervous system doesn't negotiate. It responds to inputs: breath, temperature, movement, safety. Give it the inputs, and it will do what it was designed to do. The bear isn't real. Your body just needs you to prove it.
Sources
- Harnessing Non-Invasive Vagal Neuromodulation: HRV Biofeedback and SSP for Cardiovascular and Autonomic Regulation - Medicine International, 2025
- Benefits from One Session of Deep and Slow Breathing on Vagal Tone and Anxiety in Young and Older Adults - Scientific Reports
- Global Wellness Summit Releases 10 Wellness Trends for 2026 - Global Wellness Institute
- A Clinician's Perspective on the Polyvagal Controversy - Psychology Today, 2026

