Most sleep advice boils down to "get seven to nine hours." It is a range so wide it barely qualifies as guidance. A new study published in BMJ Open Diabetes Research & Care just sharpened that window considerably. Researchers analyzing data from 23,475 American adults found that sleeping exactly 7 hours and 19 minutes per night was associated with the lowest risk of insulin resistance, the metabolic condition that precedes type 2 diabetes. Sleep less, and your blood sugar regulation suffered. Sleep more, and it suffered again.
The finding is built on 14 years of data from the National Health and Nutrition Examination Survey (NHANES), one of the most comprehensive health datasets in the United States, and it comes with a twist about weekend catch-up sleep that may change how you think about sleeping in on Saturdays.
The Number and What It Means
The research team, led by investigators from Guangxi Medical University in China, calculated a metric called the estimated glucose disposal rate (eGDR) for each participant. The eGDR is a clinical measure that reflects how efficiently your body processes glucose: higher values mean better insulin sensitivity, and lower values indicate your cells are becoming resistant to insulin's signals. Insulin resistance is the central mechanism behind type 2 diabetes, a condition that now affects roughly 37 million Americans and costs the U.S. healthcare system over $400 billion annually.
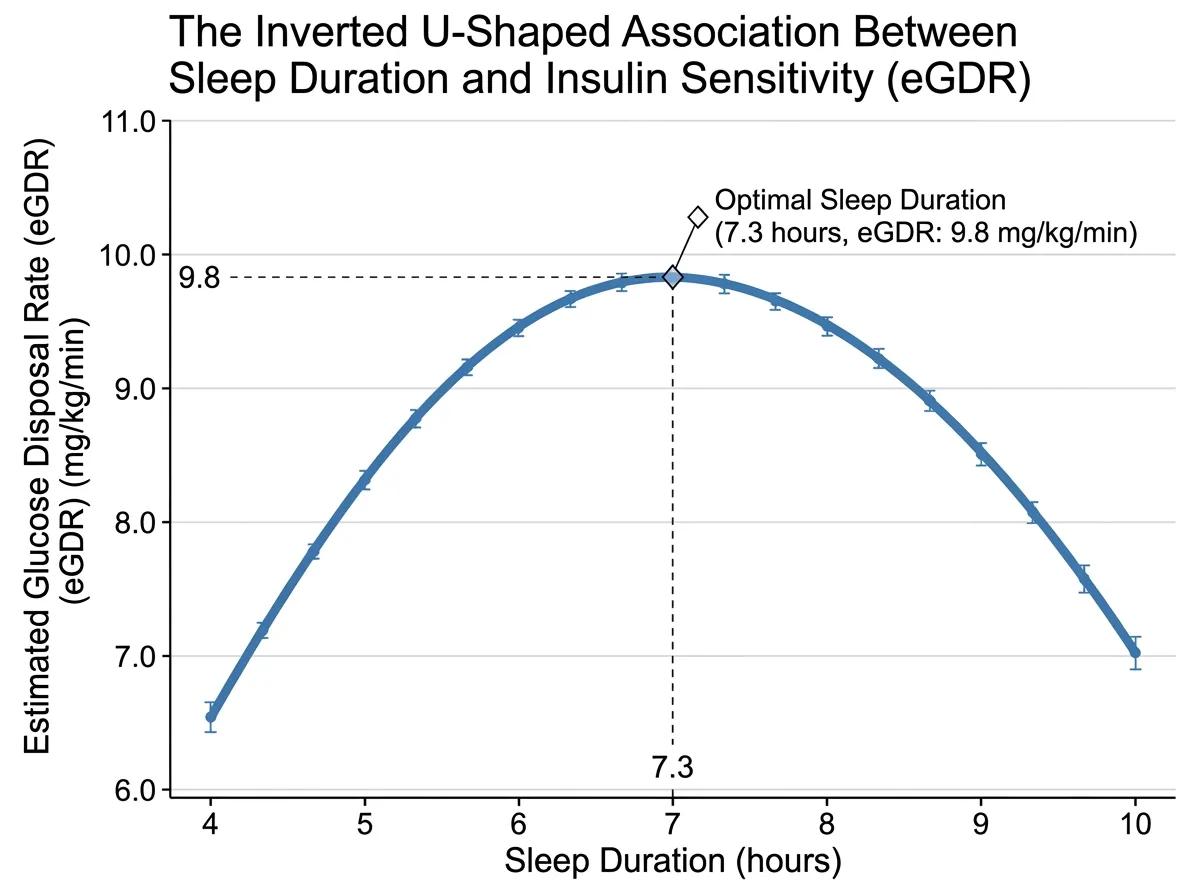
When the researchers plotted weekday sleep duration against eGDR across all 23,475 participants, the relationship formed an inverted U-curve. Glucose disposal rates climbed as sleep increased toward 7.32 hours (7 hours and 19 minutes), then declined as sleep pushed past that mark. The inflection point was sharp enough to be statistically significant and held up across multiple subgroup analyses.
The effect was strongest in three groups: women, adults aged 40 to 59, and people with a body mass index of 30 or higher. For these populations, the difference between sleeping near the sweet spot and sleeping an hour too little or too much corresponded to meaningful shifts in insulin sensitivity, the kind that shows up not just in lab values but in long-term diabetes risk.
How They Measured It
The strength of this study lies in the dataset. NHANES is a continuous survey conducted by the Centers for Disease Control and Prevention that combines interviews, physical examinations, and laboratory tests from a representative sample of the U.S. population. Participants reported their weekday and weekend sleep durations, and researchers calculated eGDR using a validated formula that incorporates waist circumference, fasting blood glucose, and blood pressure.
The team excluded participants with missing sleep data, pre-existing diabetes diagnoses, and incomplete metabolic measurements, leaving a final cohort of 23,475 adults aged 20 to 80. Of those, 10,817 had complete data on both weekday and weekend sleep duration, enabling the weekend catch-up analysis.
The use of eGDR rather than a single fasting glucose measurement is an important methodological choice. Dr. Robert Lustig, professor emeritus of pediatric endocrinology at UC San Francisco, has noted that fasting glucose alone can appear normal even when insulin resistance is already developing, because the pancreas compensates by producing more insulin. The eGDR captures a broader picture of metabolic function by integrating multiple physiological markers. "Fasting glucose is a late indicator," Lustig told MedPage Today. "By the time it is elevated, you have likely been insulin resistant for years."
The Inverted U-Curve
The inverted U relationship means that both short and long sleep are associated with worse metabolic outcomes, but through different mechanisms. The short-sleep pathway is well documented: sleep deprivation elevates cortisol, increases sympathetic nervous system activity, promotes inflammation, and directly impairs the ability of muscle and fat cells to respond to insulin. A 2023 study published in *The Lancet Diabetes & Endocrinology* demonstrated that restricting sleep to four hours per night for just five days produced a 16% decrease in insulin sensitivity in otherwise healthy young adults.
The long-sleep pathway is less intuitive but equally supported by evidence. Excessive sleep is associated with lower physical activity, disrupted circadian rhythm signaling, and in some cases may itself be a marker for underlying conditions like depression or obstructive sleep apnea that independently worsen metabolic health. Dr. Matthew Walker, professor of neuroscience at UC Berkeley and author of Why We Sleep, has described the relationship as "a Goldilocks zone where the metabolic system functions optimally, neither overstimulated by sleep deprivation nor understimulated by excessive time in bed."
The 7-hour-and-19-minute inflection point is strikingly precise, but the researchers caution against interpreting it as a universal prescription. Individual variation in sleep need is influenced by genetics, age, physical activity levels, and overall health status. The number represents a population-level optimum, not a personal target. That said, it aligns closely with previous research. A 2022 meta-analysis in Diabetes Care covering over 1 million participants across 36 studies found that seven hours of sleep was consistently associated with the lowest type 2 diabetes risk.

The Weekend Catch-Up Paradox
The study's most surprising finding involves weekend sleep. Among participants who slept less than 7.32 hours on weekdays, getting up to two additional hours of sleep on weekends was associated with improved eGDR values. In other words, catching up on sleep partially compensated for the weekday deficit, at least in terms of insulin sensitivity.
But here is the catch: for participants who already slept 7.32 hours or more on weekdays, weekend catch-up sleep was associated with worse glucose metabolism, not better. Sleeping nine or ten hours on Saturday didn't provide a metabolic bonus. It moved the needle in the wrong direction.
This finding adds nuance to the ongoing debate about sleep debt. Previous research has been mixed on whether weekend catch-up sleep can offset the health consequences of chronic short sleep. A widely cited 2018 study in the Journal of Sleep Research found that weekend recovery sleep partially restored performance metrics after sleep restriction, but a 2019 study in Current Biology concluded that weekend catch-up sleep failed to prevent metabolic dysregulation. The new BMJ data suggests the answer may depend on which side of the optimal threshold you fall on: catch-up sleep helps the short sleepers but harms those who were already sleeping enough.
Why Sleep Wrecks Blood Sugar: The Metabolic Chain Reaction
The biological link between sleep and insulin resistance runs through at least four interconnected pathways, and understanding them explains why the dose-response curve is so steep on both sides of the optimum.
The first pathway is cortisol. Sleep deprivation raises evening cortisol levels by 37-45%, according to research from the University of Chicago's sleep lab led by Dr. Eve Van Cauter. Cortisol directly antagonizes insulin by triggering gluconeogenesis in the liver, essentially telling your body to produce more glucose at exactly the time when it should be clearing it from the blood. This creates a paradox where you are simultaneously more insulin resistant and awash in extra glucose.
The second pathway is inflammation. Even a single night of four-hour sleep increases circulating levels of TNF-alpha, IL-6, and C-reactive protein, all inflammatory markers that interfere with insulin receptor signaling. Chronic low-grade inflammation is now recognized as one of the primary drivers of insulin resistance, and chronic short sleep sustains it.
The third pathway involves the autonomic nervous system. Sleep deprivation shifts the balance toward sympathetic (fight-or-flight) dominance, which raises heart rate, blood pressure, and catecholamine levels. Catecholamines directly impair glucose uptake in skeletal muscle, the tissue responsible for disposing of roughly 80% of glucose after a meal. This is why post-meal walking can be so effective: it activates skeletal muscle glucose uptake through a pathway that bypasses insulin entirely.
The fourth pathway is appetite dysregulation. Short sleep increases ghrelin (the hunger hormone) and decreases leptin (the satiety hormone), promoting overconsumption of high-carbohydrate foods. Over time, this caloric surplus contributes to visceral fat accumulation, which further amplifies insulin resistance. The relationship becomes cyclical: poor sleep makes you eat more, eating more makes you gain visceral fat, and visceral fat makes your sleep worse through increased risk of sleep apnea.
What the Research Tells Us
The BMJ study does not prove that sleeping exactly 7 hours and 19 minutes will prevent diabetes. It is an observational study, which means it identifies an association, not a causal mechanism. Participants who sleep the optimal amount may also exercise more, eat better, or have fewer underlying health conditions. The researchers adjusted for many confounders, including age, sex, BMI, physical activity, and smoking status, but observational studies cannot eliminate all sources of bias.
What the study does provide is a more precise target than the standard seven-to-nine-hour recommendation, backed by one of the largest datasets ever assembled on sleep and metabolic health. It also provides the first large-scale evidence that weekend catch-up sleep has a differential metabolic effect depending on baseline sleep duration, a finding that should inform how clinicians counsel patients about sleep timing and individual circadian patterns.
If you are consistently sleeping less than seven hours and suspect your blood sugar management is suffering, the practical steps are well supported by evidence. Keep a consistent sleep and wake time, even on weekends. Limit caffeine after 2 PM. Cool your bedroom to 65-68 degrees Fahrenheit. And if you are relying on weekend catch-up sleep, understand that it may help, but it is not a free pass. The metabolic system rewards consistency above almost everything else.
If you are experiencing symptoms of insulin resistance, such as persistent fatigue, increased thirst, frequent urination, or darkened patches of skin, consult a licensed healthcare professional. These strategies support metabolic health but do not replace medical evaluation or treatment.
Sources
- 7 hours 18 mins may be optimal sleep length for avoiding type 2 diabetes precursor - Medical Xpress, March 2026
- Diabetes: Study finds optimal sleep amount for insulin resistance - Medical News Today, March 2026
- Seven hours sleep linked to lower insulin resistance risk - News Medical, March 2026
- Optimal Sleep Length Identified to Ward Off Insulin Resistance - Gastroenterology Advisor, March 2026
- Diabetes: About 7.5 Hours of Sleep Each Night May Help Lower Your Risk - Healthline, March 2026

