The most promising weight loss compound in years didn't come from a pharmaceutical lab. It came from the blood of a 20-foot snake.
Researchers at Stanford University and the University of Colorado Boulder have identified a molecule called pTOS that suppresses appetite as effectively as drugs like Ozempic and Wegovy, but through a completely different mechanism. Instead of slowing the stomach to reduce hunger (the approach that causes the nausea, bloating, and vomiting that plague GLP-1 drug users), pTOS travels directly to the brain and flips a switch in the hunger control center. The study, published in Nature Metabolism, found the compound by studying one of the most extreme eaters on the planet: the Burmese python.
What Happens Inside a Python After Dinner
Burmese pythons are metabolic extremists. They can go weeks or even months without eating, then swallow prey whole and spend the next several days digesting it. During that post-meal window, their metabolism surges, their organs literally grow in size, and their blood chemistry transforms.
Dr. Jonathan Long, an associate professor of pathology at Stanford, and Professor Leslie Leinwand, a distinguished biologist at CU Boulder, had been studying this feast-and-famine cycle for years. They wanted to know what molecular signals tell a python's body that it's time to stop being hungry and start processing food.
The answer was a metabolite called para-tyramine-O-sulfate, or pTOS. After a large meal, pTOS levels in python blood spike by a factor of 1,000. The molecule is produced when specialized gut bacteria break down tyrosine, a common amino acid found in dietary protein. In pythons, this bacterial process happens on a massive scale because the meals themselves are massive.
"We were looking at what changes most dramatically in the blood after feeding," Long explained in a Stanford press release. The thousand-fold spike in pTOS immediately stood out from every other metabolite the team measured.
A Different Path to the Brain
Here's where things get interesting for anyone who has ever felt queasy on Ozempic.
GLP-1 receptor agonists, the drug class that includes semaglutide (Ozempic, Wegovy) and tirzepatide (Zepbound, Mounjaro), reduce appetite primarily by slowing gastric emptying. Food sits in the stomach longer, which triggers satiety signals but also causes the gastrointestinal side effects that many users struggle with. Nausea affects roughly 40% of people starting semaglutide. Some experience vomiting, constipation, or abdominal pain severe enough to discontinue treatment.
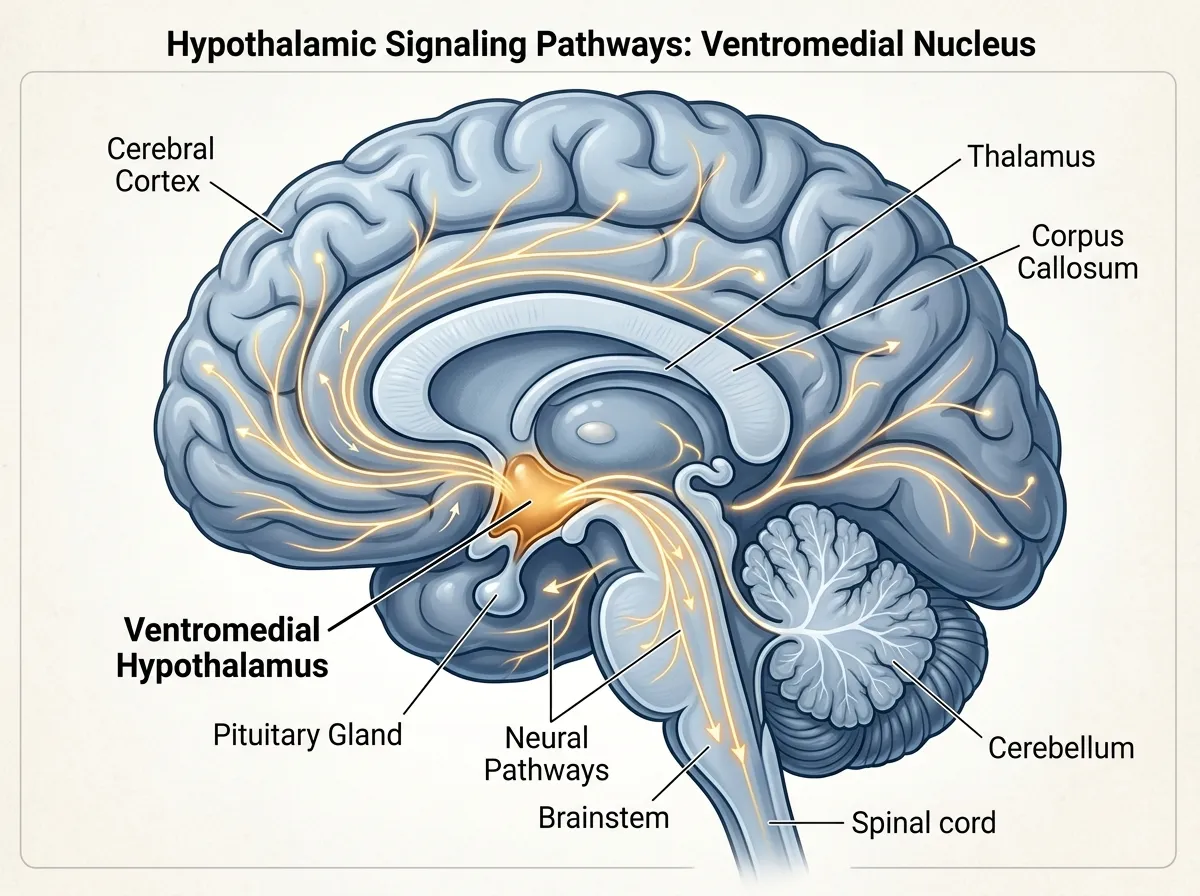
pTOS takes a different route entirely. When the researchers injected it into obese mice, they found that it traveled to the brain and activated a specific cluster of neurons in the ventromedial hypothalamus, a region long known to regulate hunger and energy balance. The compound did not alter stomach emptying at all. The mice simply ate less because their brains registered fullness through a pathway that GLP-1 drugs don't touch.
This distinction matters enormously. The GLP-1 drug market is projected to exceed $100 billion by 2030, but patient adherence remains a problem. A substantial number of patients stop taking GLP-1 medications within the first year, often because of persistent side effects. A compound that achieves similar appetite suppression without the stomach-related misery could reach the large population of people who want the benefits of these drugs but can't tolerate the costs.
28 Days, 9% Body Weight, Zero Nausea
The mouse results were striking. Over a 28-day course of daily pTOS injections, obese mice lost 9% of their body weight. They ate less voluntarily, with no signs of the gastrointestinal distress that GLP-1 drugs cause in rodent models. Their food intake dropped steadily, and the weight loss tracked consistently throughout the trial rather than plateauing early.

For context, semaglutide typically produces 12-15% body weight loss in human clinical trials over 68 weeks. A 9% reduction in 28 days in mice is not directly comparable (mice metabolize drugs differently, and the dosing timeline was compressed), but it signals that pTOS is in the same pharmacological neighborhood as the current market leaders. The mechanism's novelty, not its raw potency in mice, is what has researchers excited.
Skip Maas, a PhD candidate at CU Boulder who worked on the python metabolism side of the study, noted that the absence of GI effects was consistent across multiple dosing protocols. "We saw no evidence of delayed gastric emptying, no changes in intestinal motility," Maas said. "The appetite reduction was happening upstream of the gut."
You Already Produce This Molecule
Perhaps the most surprising finding: humans already make pTOS. While laboratory mice don't naturally carry the molecule in their blood, human studies show that we do. After a large meal, human pTOS levels rise by a factor of two to five.
That's a far cry from the thousand-fold spike in python blood, but it suggests the pathway is already wired into human physiology. Our gut bacteria already convert dietary tyrosine into pTOS. Our brains already have the receptors. The signal just operates at a much lower volume.
This raises practical questions that the researchers are already exploring. Could dietary changes, specifically protein-rich meals that provide abundant tyrosine, naturally boost pTOS production? Could targeted probiotics containing the right bacterial strains amplify the effect? Or would a synthetic version of pTOS, delivered as a pill or injection, be necessary to reach therapeutically meaningful levels?
Long and Leinwand have formed a startup called Arkana Therapeutics to pursue the clinical development path. The company is exploring applications beyond weight loss, including sarcopenia, the progressive loss of muscle mass that affects millions of older adults. If pTOS modulates energy balance at the hypothalamic level, it could potentially influence how the body allocates resources between fat storage and muscle maintenance.
What the Research Tells Us
This is early-stage science, and the gap between a promising mouse study and an FDA-approved drug is measured in years and billions of dollars. The compound needs toxicology studies, pharmacokinetic profiling, Phase I safety trials, and the large randomized controlled studies that GLP-1 drugs have already completed. Many promising metabolites have failed at one of those stages. If you're currently taking or considering GLP-1 medications, this research doesn't change the clinical picture today. Consult your physician before making any changes to existing weight management regimens.
But the finding is significant for two reasons that extend beyond any single compound. First, it demonstrates that appetite suppression can occur through a non-GLP-1 pathway with a fundamentally different side effect profile. That opens an entire new lane of drug development for obesity, a disease that affects more than 40% of American adults according to the CDC. Second, it validates the approach of studying extreme animal physiology to discover human therapeutic targets, a field sometimes called "evolutionary pharmacology" that has historically been underfunded relative to its potential.
The growing body of research connecting metabolic health to systems once considered unrelated, from sleep architecture to autonomic nervous system regulation, keeps reinforcing a consistent message: the biology of weight, hunger, and energy is far more complex than calorie arithmetic. pTOS adds a new variable to that equation, one that was hiding in plain sight inside the blood of a snake that eats once a month.
For the millions of people who can't use GLP-1 drugs because of side effects, cost, or supply constraints, the python's metabolic playbook offers a credible reason to pay attention.
Sources
- Pythons' feast-and-famine life hints at new weight-loss pathway - Stanford Medicine
- Potent Ozempic Alternative Hiding in Python Blood - ZME Science
- Python blood suppresses appetite without the side effects of drugs like Ozempic - The Brighter Side of News
- University of Colorado study finds python blood could lead to weight loss drug - CBS Colorado

